Irene H. Heijink
Resume
Full Professor since 2022
Chair: Cellular and Molecular Lung Pathology
Professor, Tenure-track Associate Professor, University of Groningen, The Netherlands, 2015 – 2022
Lead of EXPIRE Group, Departments of Pulmonology and Pathology & Medical Biology, University of Groningen, The Netherlands, 2013 –
Tenure Track, University of Groningen, University Medical Center Groningen, The Netherlands, 2011 – 2015
Post-doctoral position, University of Groningen, The Netherlands, 2009
PhD, Departments of Allergology, Hematology and Pulmonology, University of Groningen, The Netherlands, 2004
Thesis title: Dysregulation of T cell activity in asthma; role of the β2-adrenergic/cAMP system
BSc, University of Groningen, Medical Biology, Faculty of Mathematics and Natural Sciences, 1998
Research
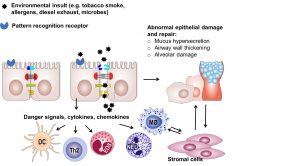
The main focus of my research is the damage and repair of the immunological mucosal barrier in lung disease. After my initial interest in the regulation of immune responses and interaction between T cells and the structural epithelial cells of the lung, my focus shifted towards the role of the damaged airway epithelial barrier as a major driver of the pathogenesis of asthma and COPD. I studied a novel role of airway epithelial barrier dysfunction in these obstructive lung diseases, showing that loss of epithelial barrier function is critical in the decision towards immunity, and that epithelial-to-mesenchymal transition may drive tissue remodeling in these diseases. Additionally, my team and I were one of the first to show that airway epithelial cells from COPD patients display mitochondrial dysfunction and that this contributes to abnormal epithelial repair.
The research of my team and I is mainly performed using molecular approaches and cellular models in a highly translational setting. Close collaboration with clinicians and pathologists has enabled a unique biobank of lung epithelium and mesenchymal stromal cells for the use of advanced, patient-specific models, including the recently set-up human airway and alveolar organoid models, airway-on-chip model, and organ-on-chip models. These advanced 3D models support our understanding of the mechanisms underlying abnormal lung epithelial repair and regeneration and allow us to study dysregulated interactions between epithelial cells and their lung microenvironment, including immune cells, stromal cells, and the extracellular matrix. The final goal is to gain more insight into novel, personalized therapeutic strategies to repair the damaged epithelial barrier in lung disease.
I lead various research consortia, including the NWO-Perspectief-funded project RecovAir and projects supported by funding from, e.g., the Dutch Lung Foundation-Health~Holland and ZonMW-Open. I was a co-founder of the large national consortium P4O2 – precision medicine for more oxygen. I have a broad international network, including collaborations with the University of Ghent, the University of British Columbia (Vancouver, Canada), and the University of Sydney (Australia). Furthermore, I am the program leader of the Groningen Research Institute for Asthma and COPD (GRIAC) and the outgoing head of the European Respiratory Society (ERS) Assembly 3 (Basic and Translational Sciences).
Samarelli, AV, Tonelli, R, Heijink, I, Martin Medina, A, Marchioni, A, Bruzzi, G et al.. Dissecting the Role of Mesenchymal Stem Cells in Idiopathic Pulmonary Fibrosis: Cause or Solution. Front Pharmacol. 2021;12 :692551. doi: 10.3389/fphar.2021.692551. PubMed PMID:34290610 PubMed Central PMC8287856.
Pouwels, SD, Wiersma, VR, Fokkema, IE, Berg, M, Ten Hacken, NHT, van den Berge, M et al.. Acute cigarette smoke-induced eQTL affects formyl peptide receptor expression and lung function. Respirology. 2021;26 (3):233-240. doi: 10.1111/resp.13960. PubMed PMID:33078507 PubMed Central PMC7983955.
Faura Tellez, G, Willemse, BW, Brouwer, U, Nijboer-Brinksma, S, Vandepoele, K, Noordhoek, JA et al.. Protocadherin-1 Localization and Cell-Adhesion Function in Airway Epithelial Cells in Asthma. PLoS One. 2016;11 (10):e0163967. doi: 10.1371/journal.pone.0163967. PubMed PMID:27701444 PubMed Central PMC5049773.
Ojo, O, Lagan, AL, Rajendran, V, Spanjer, A, Chen, L, Sohal, SS et al.. Pathological changes in the COPD lung mesenchyme–novel lessons learned from in vitro and in vivo studies. Pulm Pharmacol Ther. 2014;29 (2):121-8. doi: 10.1016/j.pupt.2014.04.004. PubMed PMID:24747433 .
Heijink, I, van Oosterhout, A, Kliphuis, N, Jonker, M, Hoffmann, R, Telenga, E et al.. Oxidant-induced corticosteroid unresponsiveness in human bronchial epithelial cells. Thorax. 2014;69 (1):5-13. doi: 10.1136/thoraxjnl-2013-203520. PubMed PMID:23980116 .
Lo Tam Loi, AT, Hoonhorst, SJ, Franciosi, L, Bischoff, R, Hoffmann, RF, Heijink, I et al.. Acute and chronic inflammatory responses induced by smoking in individuals susceptible and non-susceptible to development of COPD: from specific disease phenotyping towards novel therapy. Protocol of a cross-sectional study. BMJ Open. 2013;3 (2):. doi: 10.1136/bmjopen-2012-002178. PubMed PMID:23377993 PubMed Central PMC3586075.
Search PubMed2025 Dutch National Growth Fund (NGF) consortium Ombion-CPBT (Centre for Animal-free biomedical translation). Role: co-applicant. Total funding: €124 M; to UMCG: €4,4 M).
2022 NWO/TTW Perspectief consortium grant – RecovAir: REpairing lung damage via reCOVery of stromal heAlth to restore respIRatory function. Role: main applicant and program leader. Funding: €3,758,855.
2022 Longfonds PPS allowance Health~Holland grant – A novel stRatEgy to improve STRomal health in chronic obstrUCTive pUlmonaRy diseasE (COPD): paving the way for lung tissue regeneration. Post-doc position. Role: Main applicant and project leader. Funding: €428,198.
2021 ZonMW Open Competition grant Targeting mitochondrial dysfunction to enhance lung tissue repair in COPD; muscles to the rescue (MitoReg). Role: Main applicant and project leader. Funding: €750,000.